The name by which this disease is known alludes to the wolf -lupus in Latin- because of the destructive injuries that can bring to mind the bites of this animal. It is possible that in the beginning the name did not refer to a particular disease, but rather to any ulcerated injury with the destruction of tissue.
Although this name has been attributed to Paracelsus (1493-1541), Giovanni Manardi (1462-1536) had previously referred to some ulcers on the leg, which destroyed the surrounding area, using the comparison with a bite of hungry wolf.
Paracelsus, somewhat younger than Manardi, may have taken this graphic denomination from him, since he (Paracelsus) frequently speaks about lupus, fluently and as if dealing with something already known which did not need further explanation. As far as he was concerned, lupus was a cutaneous injury that "devoured" the excess blood, for which reason he suggested treating it with bleeding.
Rudolf Virchow's keen historical curiosity led him to make a great effort towards establishing the origin of the term and to investigate ancient sources. According to his conclusions it might have been a popular term used in the Middle Ages, and, having caught on, later became more generalized and entered the language of Medicine, thereby preceding Manardi and Paracelsus and their usage. One of the texts that he found, attributed to the German Johann Tollat von Vorchenberg, written at the beginning of the 15th century, said textually:
...for the wolf and for cancer, caprifolin...
Another text referred to by Rudolf Virchow (1821-1902) is older still. It dates back to the end of the 13th century and is a treatise on surgery by Roger de Palma, of the
Sometimes lupus arises in the thighs and the lower legs (and is) distinguished from cancer from the symptoms mentioned above.
Nevertheless, no passage has been found that reveals the distinction between lupus and cancer. What is clear, however, is that from Roger to Manardi, lupus is spoken of as a typical complaint affecting the lower extre mities. So, in those times, the term lupus would not refer, as it would later, to a disease of the nose and face. As Virchow already stated, this denomination was applied in a very diverse and vague way in the Middle Ages. It was Virchow himself who showed that Hans von Gersdorf was one of the first medical writers that referred to a facial disorder using the word lupus:
mities. So, in those times, the term lupus would not refer, as it would later, to a disease of the nose and face. As Virchow already stated, this denomination was applied in a very diverse and vague way in the Middle Ages. It was Virchow himself who showed that Hans von Gersdorf was one of the first medical writers that referred to a facial disorder using the word lupus:
Leprosy is more clearly recognized in the nose, where it shows well-defined symptoms. Sometimes it is a
lso called wolf because it can contaminate all of a man's limbs as does cancerous lupus
In short, the prevailing idea up to the end of the 16th century, inherited from the
However, there are indications that what we know today as lupus erythematosus was a disease that also existed in antiquity, even before the discovery of
What is lupus?
Lupus is a chronic, autoimmune disease that can damage any part of the body (skin, joints, and/or organs inside the body). Chronic means that the signs and symptoms tend to last longer than six weeks and often for many years. In lupus, something goes wrong with your immune system, which is the part of the body that fights off viruses, bacteria, and other germs (“foreign invaders,” like the flu). Normally our immune system produces proteins called antibodies that protect the body from these invaders. Autoimmune means your immune system cannot tell the difference between these foreign invaders and your body’s healthy tissues (“auto” means “self”). In lupus, your immune system creates autoantibodies , which attack and destroy healthy tissue. These autoantibodies cause inflammation, pain, and damage in various parts of the body.
When people talk about “lupus,” they usually mean systemic lupus erythematosus. This is the most common type of lupus. Studies suggest that more than 16,000 new cases are reported annually across the country.
Although lupus can affect almost any organ system, the disease, for most people, affects only a few parts of the body. For example, one person with lupus may have swollen knees and fever. Another person may be tired all the time or have kidney trouble. Someone else may have rashes.
Normally, lupus develops slowly, with symptoms that come and go. Women who get lupus most often devel
op symptoms and are diagnosed between the ages of 15 and 45. But the disease also can develop in childhood or later in life.
For most people, lupus is a mild disease. But for others, it may cause serious problems. Even if your lupus symptoms are mild, it is a serious disease that needs treatment. It can harm your organs and put your life at risk if untreated.
Although the term “lupus” commonly refers to SLE, this is only one type of the disease. There are other, less common types of lupus:
- Discoid lupus erythematosus, also called DLE, mainly affects the skin. A red rash may appear. Or, the skin on the face, scalp, or elsewhere may become scaly or change color. Sometimes DLE causes sores in the mouth or nose. A doctor will remove a small piece of the rash or sore and look at it under a microscope to tell if someone has DLE. If you have DLE, there is a small chance that you will later get SLE. There is no way to know if someone with DLE will get SLE.
- Drug-induced lupus is a lupus-like disease caused by certain prescription drugs. The symptoms of drug-induced lupus are similar to those of systemic lupus, but only rarely will any major organs be affected. Symptoms can include: joint pain, muscle pain, and fever. Symptoms are mild for most people. Most of the time, the disease goes away when the medicine is stopped. More men get this type of lupus because the drugs with the highest risk of causing it are used to treat heart conditions that are more common in men; however, not everyone who takes these drugs will develop drug-induced lupus. The drugs most commonly connected with drug-induce d lupus are procainamide (Pronestyl®, Procanbid®) and hydralazine (Apresoline®; also, hydralazine is an ingredient in Apresazide® and Bidil®).
- Neonatal lupus is a rare condition that affects infants of women who have lupus and is caused by certain antibodies from the mother acting upon the infant in the womb. At birth, the infant may have a skin rash, liver problems, or low blood cell counts, but these symptoms disappear completely after several months with no lasting effects. Some infants with neonatal lupus can also have a serious heart defect. With proper testing, physicians can now identify most at-risk mothers, and the infant can be treated at or before birth. Most infants of mothers with lupus are entirely healthy.
Anyone can get lupus. But 9 out of 10 people who have lupus are women. African American women are three times more likely to get lupus than white women. Lupus is also more common in Hispanic/Latina, Asian, and Native American women.
African Americans and Hispanics/Latinos tend to get lupus at a younger age and have more symptoms, including kidney problems. Lupus also tends to be more severe in these ethnic groups. For example, African Americans with lupus have more problems with seizures and strokes. Hispanic/Latino patients have more heart problems. Scientists believe that genes play a role in how lupus affects these ethnic groups.
Why is lupus a concern for women?
Nine out of 10 people who have lupus are women. And lupus is most common in women of childbearing years. Having lupus increases your risk of developing other health problems that are common in women. It can also cause these diseases to occur earlier in life:
- Heart disease. When you have lupus you are at increased risk for the main type of heart disease, called coronary artery disease (CAD). This is partly because people with lupus have more CAD risk factors, which may include: high blood pressure (hypertension), high cholesterol levels, type 2 diabetes, and an inactive lifestyle due to fatigue, joint problems, and/or muscle pain. Heart disease is the number one killer of all women. But, women with lupus are 50 times more likely to have chest pain or a heart attack than other women of the same age.
- Osteoporosis. Women with lupus have more bone loss and breaks than other women. This is thought to happen because some medicines used to treat lupus cause bone loss. Bone loss also may occur as a direct result of the disease. Also, pain and fatigue can keep women with lupus from exercising. Keeping active is an important way to keep bones healthy and strong.
The cause of lupus is not known. More than one factor is likely to play a role in getting lupus. Researchers are looking at these factors:
- Environment (Sunlight, stress, certain medications, and viruses might trigger symptoms in people who are prone to getting lupus.)
- Hormones (Lupus is more common in women during childbearing years.)
- Problems with the immune system
What are the symptoms of lupus?
The signs of lupus differ from person to person. Some people have just a few symptoms; others have more. Lupus symptoms also tend to come and go. Lupus is a disease of flares (the symptoms worsen and you feel ill) and remissions (the symptoms improve and you feel better).
Common signs of lupus are:
- joint pain and stiffness, with or without swelling
- muscle aches and pains
- fever with no known cause
- feeling very tired
- skin rashes
- anemia (too few red blood cells)
- trouble thinking, memory problems, confusion
- kidney problems with no known cause
- chest pain when taking a deep breath
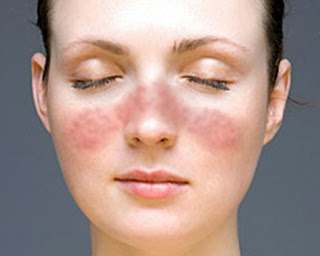
- butterfly-shaped rash across the nose and cheeks
- sun or light sensitivity
- hair loss
Less common symptoms include:
- blood clots
- purple or pale fingers or toes from cold or stress
- seizures
- sores in the mouth or nose (usually painless)
- severe headache
- dizzy spells
- "seeing things", not able to judge reality
- feeling sad
- strokes
The Other Symptoms of Lupus
The symptoms of SLE come on in waves, called flares or flare-ups. In between flares, patients may have almost no symptoms. Almost every SLE patient suffers from general discomfort, extreme fatigue, fever, and weight loss at some point. In addition to these general symptoms, SLE produces different symptoms in different body systems.
Skin
People with SLE tend to be very sensitive to sunlight. Being in the sun for even a short time can cause a painful rash. Some people even get a rash from fluorescent lights at work.
Muscles and Bones
In its late stages, SLE can cause areas of bone tissue to die, called osteonecrosis.. Osteonecrosis can cause serious disability. It can be caused at least in part by using high doses of corticosteroids over a long time. Corticosteroids help control the symptoms of SLE.
Kidneys
Nervous System
Membranes
Digestive System
Lungs
- Inflammation of the lungs, called Lupus pneumonitis, can come on suddenly or slowly. It has many of the same symptoms of pneumonia.
- A hemorrhage (burst blood vessel) can occur in the lungs.
- A blood clot can form in the artery going to the lungs.
- The blood vessels in the lungs can begin to contract.
- Shrinking lung syndrome involves scarring of the lungs due to long standing inflammation decreases the lungs' capacity to take in air. It seems that the lungs can no longer hold normal amounts of air.
Blood
You may have few of these symptoms, almost all of them, or any combination in between. The disease affects different people in very different ways. There is even a group of patients considered to have latent lupus. They have some chronic SLE symptoms, but the disease never seems to progress into true SLE.
A few patients have drug-induced lupus. In these cases, SLE symptoms come on suddenly while taking certain kinds of drugs. The symptoms are usually milder than in true SLE, and the symptoms go away when the patients stop taking the drug.
Pregnancy
Medication
Several types of drugs can be used to treat the complications of SLE. What your doctor prescribes for you will depend on your symptoms.
- Nonsteroidal anti-inflammatory drugs (NSAIDs) are used to treat muscle, bone, and joint pain, and mild cases of serositis (inflammation of internal membranes). They may also be used for fevers.
- Corticosteroids are used in many forms. Creams are rubbed into rashes, and oral or intravenous forms are used to treat flare-ups and to keep the disease under control. Corticosteroids can be injected directly into painful arthritic joints. These drugs are very toxic, howevehydroxychloroquine, chloroquine, and quinacrine) work to manage the skin problems of SLE. They can also help treat other symptoms. These drugs can hurt your eyes. As a preca
- Methotrexate in low weekly doses can help manage arthritis, rashes, serositis, and other symptoms.
- Cyclophosphamide, given intravenously, is often used when SLE is affecting the kidneys, heart, and lungs. This is an extremely toxic drug, with many side effects. Patients often experience severe nausea and vomiting and almost total hair loss. The hair does grow back, even when patients must continue taking the drug.
- Azathioprine can be used instead of cyclophosphamide to treat kidney disease. Doctors consider it less effective, but it is also far less toxic. It can also be used instead of steroids.
SLE progressively damages the kidneys over time. In late stages of the disease, kidney failure requires dialysis or kidney transplants.
SLE is a very serious disease. Its effects on the kidneys, heart, and lungs can cause many long-term problems. Although doctors now have better ways to help you live with SLE, there are not many options to help prevent or reverse the damage to your organs.
Taken from:
www.womenshealth.gov
www.eorthopod.com
www.bium.univ-paris5.fr